
The Patient Advice System
The Patient Advice System
How can we connect hospital patients with each other to share advice and support?
Timeline: 4 years (1-3 months per study)
Team: 4 researchers, 1 clinician, 2 hospital staff
Methods: survey, interviews, card sorting, technology probe, affinity diagramming, qualitative analysis, descriptive statistical analysis
Opportunity
Exchanging health advice with patient-peers can have several benefits, such as increased knowledge, empowerment, and improved health outcomes. Most patient-peer technologies are designed for patients with chronic conditions for use in non-hospital settings. We don’t know what design opportunities and constraints exist for patient-peer technologies in the hospital.
Goals
My goals for this project were to:
Understand what needs hospital patients might have to connect with each other and share advice.
Identify opportunities, barriers, and design recommendations for technologies to facilitate this support.
Explore how patients might use a peer support technology during their hospital stay.
Determine what impact a peer support technology could have on a patient’s hospital experience.
methods
First, to understand what needs hospital patients might have to connect with each other, I designed and conducted a survey study with 242 patients and family members. In addition to other questions about their hospital experience, I asked what advice they would share with their fellow patients. Advice was shared by 88% of survey respondents. I reviewed the survey respondents’ advice and found many recurring themes.
Next, I decided to explore design concepts for a peer support tool in interviews with 30 hospital patients. I created cards representing hypothetical features of a peer support tool. During interviews, I had hospital patients complete a card sorting activity to share their thoughts about connecting with other patients and to share their design feedback.

In Sketch, I created these "feature cards" for a card sorting activity during interviews with hospital patients. Each card represents a hypothetical feature of a peer support tool.
findings & key insights
My qualitative analysis of the survey and interview data revealed that hospital patients have many unmet needs to connect with their peers in the hospital, such as sharing emotional support and discussing ways to prevent medical errors.
“You look online, but it’s not – it’d be nice just to have [information from peers] all together instead of searching through massive information.”
-Interview Participant #15
Most interview participants liked the idea of using a peer support tool in the hospital, but they also had privacy concerns and cognitive or physical burdens from treatment that were considered barriers to using such a tool.
Based on these findings, I identified several design recommendations for peer support tools in the hospital. Examples included:
Offer asynchronous interactions to reduce burdens of connecting with peers when feeling ill.
Have patients exert control over their privacy.
Provide easy navigation and search for relevant information and advice from peers.
outcomes & impact
To incorporate my recommendations, I iteratively prototyped low-fidelity solutions that balanced user needs and project constraints (e.g., limited technical and financial resources). I then built mid-fidelity prototypes and gathered feedback from my team.

I worked with another researcher to brainstorm feature ideas of a prototype.

After brainstorming, I created paper sketches and mockups of a peer support tool.

After sketching I built mid-fidelity prototypes, like a patient slack channel and survey to rate peer advice.
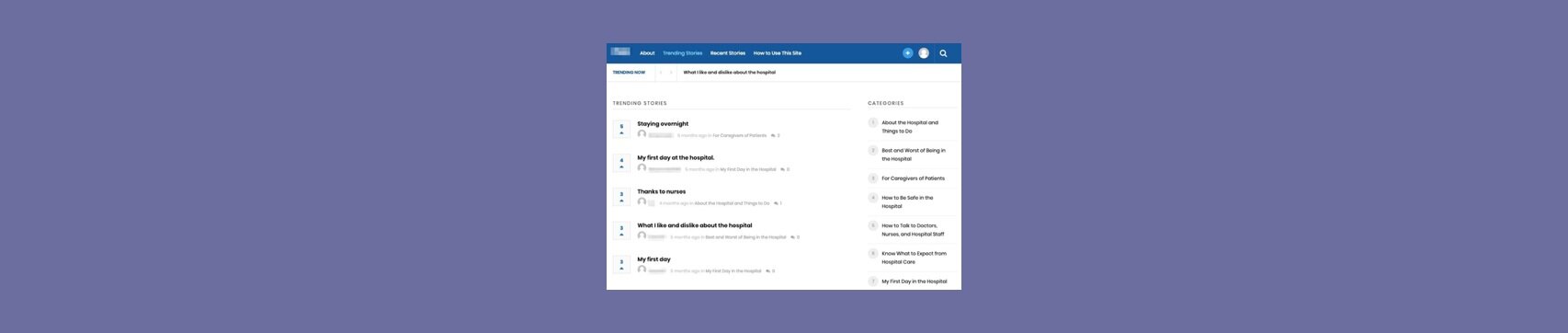
After many rounds of prototyping and pilot testing with design experts, I created a Reddit-inspired peer support tool. The tool, called The Patient Advice System (PAS), is a web-based online community for hospital patients. Here’s how it incorporates my design recommendations:
To offer asynchronous interactions, patients can post stories, comment on, and upvote stories about their hospital experiences.
To have patients exert control over their privacy, patients create their own username to interact with their peers.
To provide easy navigation, the PAS shows categories of stories for patients to easily browse related information from their peers.

Screenshot of the PAS home page after deployment concluded at one of 2 hospitals. The design was based
on the input I received from interviews and feature card sorts with hospital patients.
After creating the PAS, I studied how patients would use it in the real-world. I deployed the PAS with 30 hospital patients and conducted pre- and post-interviews to learn the use and impact of tool on their hospital stay. I also asked for patients’ feedback on its design.
I worked with a researcher on a quantitative analysis of PAS usage data and led a qualitative analysis of the pre- and post-interviews.

A research colleague and I created anonymized profiles of each PAS participant. We did a few rounds of affinity diagramming to identify usage patterns.

We analyzed many kinds of data (e.g., participant demographics, sentiment of stories) to understand the usage patterns we identified.
Patients used the PAS in a variety of ways to tell stories, connect with their peers, and demonstrate support for their peers without directly communicating. Patients who posted stories and comments shared advice on how to adjust from home to the hospital and tips for communicating with their providers.
In using the PAS, patients experienced many benefits, like successfully intervening in errors and improving their emotional wellbeing:
“It made me feel a little better about being in that situation…because I felt like I wasn’t alone and I could relate to people.”
-PAS Participant #7
These benefits were experienced by patients regardless of clinical diagnosis, prior hospital experience, and level of interaction with peers.
However, patients also had challenges using the PAS in the hospital, like not seeing frequent activity from their peers and experiencing cognitive or physical burdens that prevented them from using the tool. Based on this patient feedback, I identified more design recommendations for future versions of the PAS:
Integrate hyperlocal information
Explore AR/VR forms of patient-peer support
Provide dynamic peer support based on patient illness phases
The results of this study encouraged organizational leadership at other hospitals to explore similar peer support solutions for their patients.
My deployment procedures have been reused successfully by other researchers in at least two other technology studies in hospitals.
writing & presentations
S Haldar, Y Kim, SR Mishra, AL Hartzler, AH Pollack, W Pratt. The Patient Advice System: A Technology Probe Study to Enable Peer Support in the Hospital. Proceedings of the ACM Conference on Computer Supported Cooperative Work (CSCW 2020). [doi] [pdf] [talk]
S Haldar, SR Mishra, Y Kim, AL Hartzler, AH Pollack, W Pratt. Use and Impact of an Online Community for Hospital Patients. Journal of the American Medical Informatics Association (JAMIA 2020). [doi] [pdf]
S Haldar, AH Pollack, W Pratt. Lessons Learned from Deploying a Patient-Facing Technology Probe at a Pediatric and Adult Hospital. Workshop on Interactive Systems in Healthcare (WISH) at CHI 2019. [pdf]
S Haldar, SR Mishra, M Khelifi, AH Pollack, W Pratt. Exploring the Design of an Inpatient Peer Support Tool: Views of Adult Patients. Proceedings of the American Medical Informatics Association Annual Symposium (AMIA 2018). [pdf]
S Haldar, SR Mishra, M Khelifi, AH Pollack, W Pratt. Opportunities and Design Considerations for Peer Support in a Hospital Setting. Proceedings of the ACM Conference on Human Factors in Computing Systems (CHI 2017). [doi] [pmc] [pdf] [talk]
Opportunities and Design Considerations for Peer Support in a Hospital Setting. Workshop for Interactive Systems in Healthcare (WISH) at the American Medical Informatics Association Annual Symposium (AMIA). November 2017.
Towards the Design of an Inpatient Peer Support System. National Library of Medicine Informatics Training Conference (NLMITC). June 2017.